Traumatic Ptosis
Updated March 2025
Establishing the diagnosis
Etiology
- Traumatic ptosis can be neurogenic, aponeurotic, myogenic, or mechanical in nature.
- Pseudoptosis can mimic these phenomena.
- Iatrogenic causes account for roughly 50% of traumatic blepharoptosis (Crawford, Can J Ophthalmol 1974).
- Multiple possible factors have been suggested for ptosis after cataract surgery.
- Classically, felt to be associated with levator dehiscence
- Bridle suture, speculum placement
- Myotoxicity from anesthesia (Song, Korean J Ophthalmol 1996)
- After oculoplastic surgical procedures
- Postoperative edema or hematoma can create a mechanical ptosis.
- Trauma to levator muscle, particularly during blepharoplasty (Bernardino, Semin Ophthalmol 2002)
- Full-thickness resection can cause direct damage to levator muscle or Muller’s muscle (Altieri, Ophthalmologica 2005).
- Resection of conjunctival tumors can create a symblepharon, dragging the eyelid into a ptotic position (Bosniak, 1990).
- After administration of botulinum toxin
- Can create a self-limited ptosis with impaired levator function
- Incidence reported to be 5.4% (Henderson, Dev Ophthalmol 2008).
- After strabismus surgery
- Superior rectus advancements can result in ptosis.
- Classically, avoided with meticulous dissection (Altieri, Ophthalmologica 2005)
- Birth trauma
- Classically, thought to be related to levator dehiscence (Carruthers, J Am Acad Dermatol 2002)
- Blunt trauma (Figure 1)
- Edema of levator
- Dehiscence of levator
- Generally self-limited (Altieri, Ophthalmologica 2005)
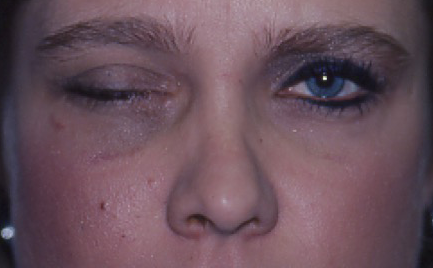
Figure 1. Blunt trauma. Courtesy Evan H. Black, MD.
- Penetrating/lacerating trauma (Figure 2)
- Occurs in setting of direct injury to the levator muscle
- Classically, immediate exploration with restoration of appropriate anatomy facilitates resolution of ptosis (Putnam, 1995)
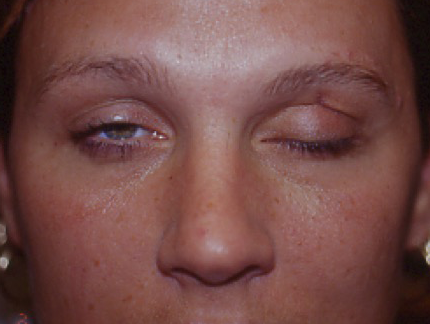
Figure 2. Lacerating trauma. Courtesy Evan H. Black, MD.
- Associated with facial fractures
- Facial fractures can result in enophthalmos, creating the appearance of ptosis (Altieri, Ophthalmologica 2005).
- With orbital roof fractures, pieces of bone can abut levator muscle, resulting in ptosis and necessitating surgical repair (Berke, Am J Ophthalmol 1971).
- Neurogenic causes
- Cranial nerve III palsy
- Typically, associated with blunt trauma to the head, most commonly due to motor vehicle accident (Fulcher, Ophthal Plast Reconstr Surg 2003)
- Generally, complete ptosis
- Ptosis often resolves after one year, although aberrant regeneration occurs in roughly 50% of cases (Lin, J Neurosurg 2013).
- Superior orbital fissure syndrome
- Involves cranial nerves III, IV, V, and VI
- Rare finding in setting of craniofacial fractures (0.3%) (Krohel, Am J Ophthalmol 1979)
- Can be associated with Lefort II or III fractures and with zygomatic complex and frontobasal skull fractures (Chen, Craniomaxillofac Trauma Reconstr 2010)
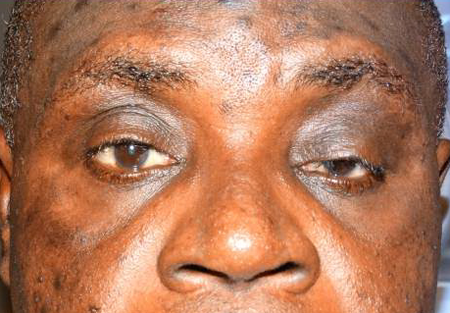
Figure 3. Courtesy Anne Barmettler, MD.
Epidemiology
- Traumatic ptosis has been reported to account for 11.2% of blepharoptosis in a tertiary care oculoplastic surgery setting (Lim, Orbit 2013).
- Intraocular surgery
- 4–12% after cataract surgery procedures (Mehat, Orbit 2012, Altieri, Ophthalmologica 2005, Boyle, 2011)
- Extracapsular cataract extraction is associated with a greater incidence of postoperative ptosis than phacoemulsification (Puvanachandra, Orbit 2010).
- 10.7% rate of ptosis after trabeculectomy alone and 12.7% rate after combined trabeculectomy/phacoemulsification (Song, Korean J Ophthalmol 1996)
History
- Mechanism of injury
- Intraocular or adnexal surgery
Clinical features
- Decreased upper eyelid marginal reflex distance
- In mechanical ptosis, evidence of eyelid edema or ecchymosis
- Neurogenic causes are associated with abnormalities of eyelid motility.
- Levator function can be decreased or normal (depending on etiology).
- Possible symblepharon
- Possible enophthalmos
- Possible entry wound or scar tissue
Testing
- Complete ophthalmic examination, ruling out evidence of intraocular trauma and ruptured globe
- Complete review of appropriate orbital and intracranial imaging
- Assess marginal reflex distance, motility, and levator function
- Check eyelid crease presence and height.
- In cases of acute trauma, assess for prolapsed orbital fat.
Risk factors
Depends on etiology
Differential diagnosis
Nontraumatic ptosis
Pseudoptosis
Patient management: treatment and follow-up
Natural history
- The management depends critically on the etiology and clinical findings, making meticulous evaluation critical.
Medical therapy
- None
Radiation
- None
Surgery
- Cases related to upper eyelid lacerations benefit from exploration and reapproximation of the levator muscle, when possible (Natl J Maxillofac Surg 2012). Delayed repair may be associated with scarring, making such interventions more difficult; surgeons should attempt repair at the time of the initial trauma (Silkiss, Adv Ophthalmic Plast Reconstr Surg 1987).
- Prolapsed orbital fat indicates that the septum has been violated.
- In cases of muscle slippage or difficulty identifying the muscle (ie severe edema), surgeons should identify Whitnall’s ligament because the levator muscle should be directly adjacent. Once suspected levator muscle is identified, the tissue can be grasped with a forceps. By asking the patient to look up, tension on the grasped tissue strongly suggests that the surgeon has located the levator muscle.
- Ptosis that is related to mechanical causes (i.e., edema) should be observed until the underlying etiology has resolved; cases of mechanical ptosis from blunt trauma recover without intervention in the majority of cases.
- Many authorities advocate waiting at least 3 months for resolution of postoperative ptosis prior to repair; the outcomes of postoperative ptosis repair are generally favorable and are generally consistent with involutional ptosis repair.
- Neurogenic ptosis
- Typically, many of these patients experience spontaneous resolution (Lin, J Neurosurg 2013).
- Consequently, surgical repair is generally delayed for one year.
Other management considerations
- None
Common treatment responses, follow-up strategies
- In cases of poor levator function (less than 5 mm), consider frontalis sling procedure.
- With better levator function, consider levator advancement.
References and additional resources
- Altieri M, Truscott E, Kingston AE. Ptosis secondary to anterior segment surgery and its repair in a two-year follow-up study. Ophthalmologica. 219(3):129-35, 2005.
- Berke RN. Surgical treatment of traumatic blepharoptosis. Am J Ophthalmol, 72: 691-8, 1971.
- Bernardino CR and Rubin PAA. Ptosis after cataract surgery. Semin Ophthalmol, 17: 144-8, 2002.
- Bosniak SL. Complications: diagnosis and treatment. Cosmetic blepharoplasty. New York: Raven, 1990.
- Boyle NS and Chang EL. Traumatic blepharoptosis. In: Cohen AJ and Weinberg DA (eds), Evaluation and Management of Blepharoptosis, New York: Springer, 2011.
- Carruthers JA, Lowe NJ, Menter MA, et al. A multicenter, double-blind, randomized, placebo-controlled study of the efficacy and safety of botulinum toxin type A in the treatment of glabellar lines. J Am Acad Dermatol, 46: 840-9, 2002.
- Chen C, Chen Y. Traumatic superior orbital fissure syndrome: Current management. Craniomaxillofac Trauma Reconstr, 3:9–16, 2010.
- Crawford JS. Ptosis as a result of trauma. Can J Ophthalmol, 9: 244-8, 1974.
- Fulcher TP and Sullivan TJ. Orbital roof fractures: management of ophthalmic complications. Ophthal Plast Reconstr Surg, 19: 359-63, 2003.
Financial disclosures
Reviewers
Lora Dagi Glass: Consultant, Ora Clinical
